Are you losing money on hearing aid claims?
TIMS Software partners with Healthcare Revenue Group, LLC to help you maximize your audiology practice revenue. If you struggle with insurance...
1 min read
 Computers Unlimited
:
Updated on November 11, 2024
Computers Unlimited
:
Updated on November 11, 2024

No One Likes Rejection
The dreaded claim rejection. No one has time for that. Chasing rejected claims is a huge time waster but it doesn't have to be that way. Whether you work in an audiology practice, university, or hospital setting, you may wear many different hats: from patient scheduling to ordering supplies, from payroll to marketing. One way to make your day run smoother is by using the right software system so you can get paid faster.
1. Insurance
When you begin with a solid foundation of insurance payors along with their ID numbers, you can quickly add them to your patient billing information. The right software should let you set up both primary, secondary, and any additional payors as necessary.
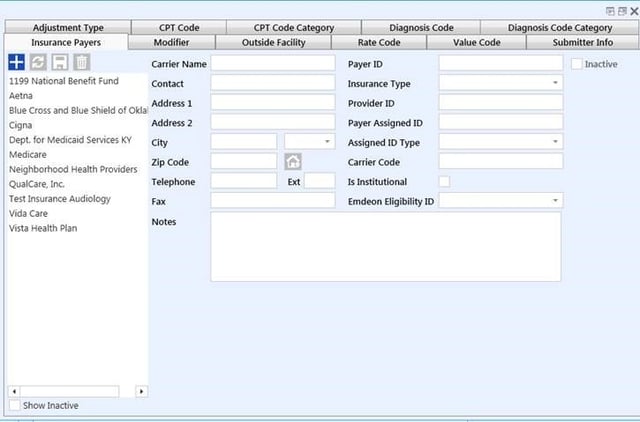 Add payors to TIMS and then easily add them to your patient claims.
Add payors to TIMS and then easily add them to your patient claims.
2. Coding
CPT codes and diagnosis codes need to be validated every year. Doing so gives you all the current coding you need for successful claim submission.
3. Data Entry
TIMS Software has a single screen that is used to collect and edit patient data during the visit. Whether you're entering demographics, insurance details, referring and primary physicians, or customized data, TIMS allows for quick and easy entry.
4. Billing
Make it easy on yourself. TIMS gives you the ability to create an Electronic Superbill, tracking every patient appointment from claims to billing. Within the Superbill process, you can quickly add the CPT and diagnosis codes. When finalized, this creates your claims submission. This allows you to electronically submit the claims (ask about the claims pricing breakdown); no paper, no going back and forth to different systems.
Need assistance processing your claims? Claim.MD is a TIMS Partner who can help.
5. Reporting
Keep track of all your claims in TIMS by checking to see if your claims were accepted at the clearinghouse or the payor. The claim status inquiry button checks the payor level status of any outstanding claims.
Last updated 7/18/24

TIMS Software partners with Healthcare Revenue Group, LLC to help you maximize your audiology practice revenue. If you struggle with insurance...

2 min read
The Right Claims Process Leads to Getting Paid Faster Want to make your claims process smoother and more efficient than ever? Upgrade to the latest...

Streamline Your Billing with TIMS Superbill Functionality!